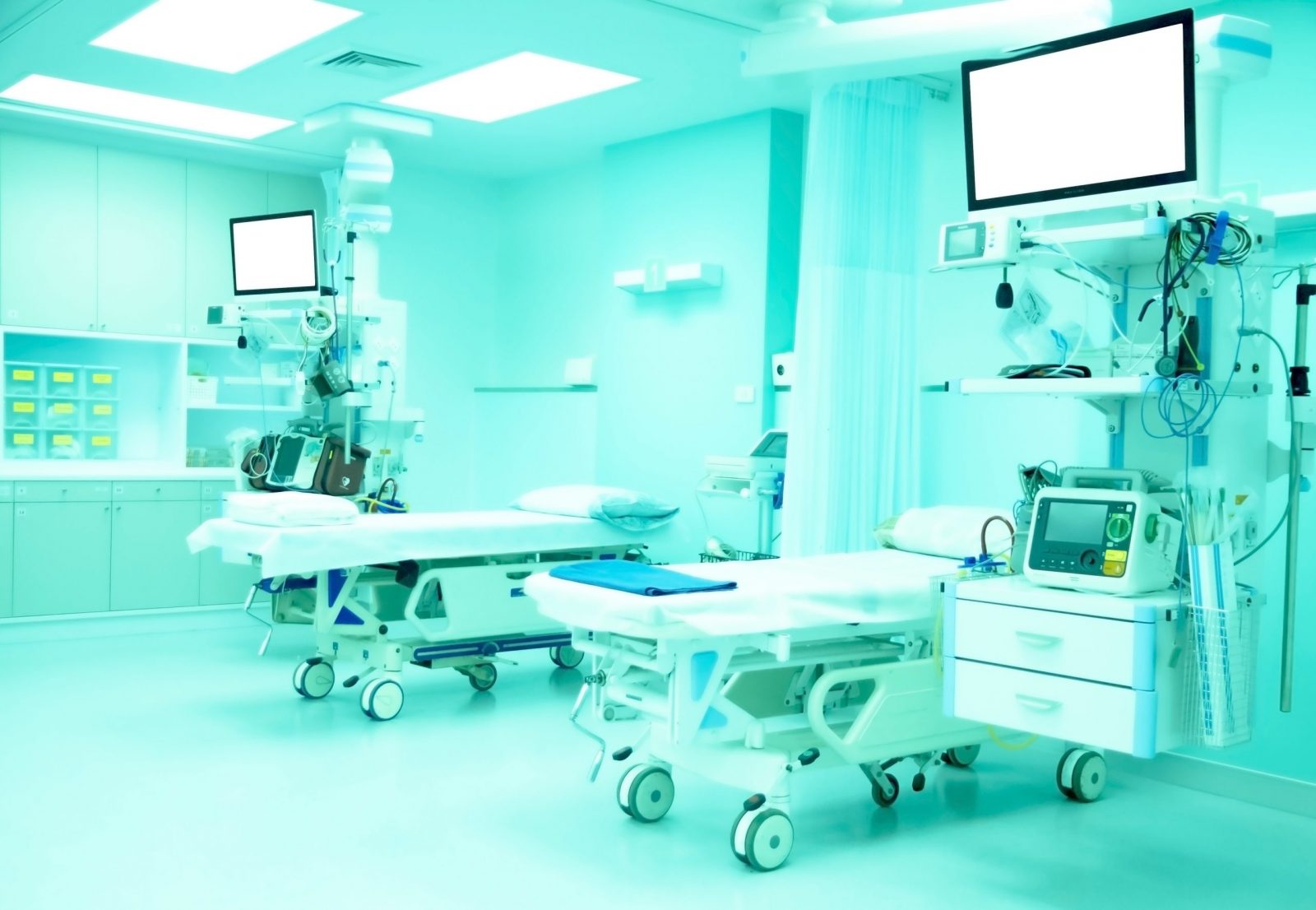
The spread of pathogenic microorganisms can occur through different vectors of transmission. These vectors including air, surfaces and water act as a bridge that transports the infectious agents directly or indirectly into humans or living organisms. It is very important to understand the differences within these routes and the differences among the pathogenic microorganisms for better infection control measures. For example, an airborne pathogen can differ from a waterborne pathogen in terms of the disease or infection they cause and their survivability characteristics. Airborne pathogens are known to primarily cause but not limited to upper respiratory tract infections such as the common cold or pneumonia, whilst water-borne pathogens can cause gastroenteritis and other diarrhoeal infections. However, some pathogens can have more than one route of transmission, as it was reported with the recent SARS-CoV-2 which showed stability as an aerosol, on surfaces and in water. This is in addition to other microorganisms such as Staphylococcus aureus, Escherichia coli, Norovirus, Salmonella spp. and Actinobacter baumannii.
During the search process, not many published articles were found addressing all the routes and vectors of transmission and their relevant microorganisms. Therefore, in this article, we will discuss in more detail the major routes of transmission and give an overall overview of the spread of a wide range of pathogenic microorganisms.
 Airborne infections
Airborne infections
Exposure of human beings to different airborne pathogens has resulted in the emergence of epidemics of respiratory infections. This airborne transmission becomes even more prevalent in healthcare settings because of overburdened hospitals and the presence of immunosuppressed patients. As we know, inhalation exposes the upper and lower respiratory tracts of humans to a variety of airborne particles and vapours. The lung is more susceptible to infection than the gastrointestinal tract as ingested microorganisms must pass through the acidic environment of the stomach before they can colonise tissue, while inhaled microorganisms are deposited directly on the moist surfaces of the respiratory tract. Talking and coughing generate bioaerosols from individuals, some of which may be infectious. The individual particle size of particulate material in bioaerosols is generally 0.3–100 µm in diameter; larger particles tend to settle rapidly and are not readily transported in the air. Virus particles are nanometer in size and vary from 20nm to 500nm, bacterial cells are approximately 1 µm in diameter, and fungal spores are >1 µm. These microorganisms can be dispersed in the air as single units but are often present as aggregate formations. The larger aggregates have different aerodynamic properties than single-cell units; therefore their dispersal may be different than single-unit particles. Aggregates of biological material also afford protection from environmental stresses such as desiccation, and exposure to ultraviolet radiation ozone and other pollutants in the atmosphere. A World Health Organization review of the evidence published in 2009 stated that viral infectious diseases can be transmitted across distances relevant to indoor environments by aerosols (i.e. airborne infections), and can result in large clusters of infection in a short period.
The most recent example is the spread of SARS-CoV-2 in the air that caused global outbreaks in different settings during the current pandemic. It was shown in the literature that SARS-CoV-2 has the ability to disperse from patients to ward vent openings, and its viral RNA was detected in ventilation exhaust filters located at least 50 m from patient room vent openings. Other viruses share similar properties in terms of stability and dispersity in the air environment such as the Influenza virus, Norovirus, MRES and SARS-COV-1 viruses. For bacteria, Mycobacterium tuberculosis is recognized for its role as the causative agent of human tuberculosis and responsible for previous outbreaks. Infected individuals can spread pathogenic bacilli when coughing, talking, speaking, laughing, and sneezing. In addition, numerous Gram-positive bacteria are usually disseminated from the skin, oral and nasal surfaces, and hair of humans. This group is more frequently isolated from air samples than Gram-negative bacteria, with Staphylococcus being the most common genus of non-endospore-forming Gram-positive bacteria isolated in indoor air samples as well as Streptococcus. On the other hand, examples of airborne Gram-negative bacteria include E. coli, Pseudomonas aeruginosa, Salmonella, Klebsiella pneumoniae, Legionella pneumophila and many others. Which all contribute to unwanted nosocomial infections such as pneumonia, bacteremia, meningitis, and other complications.
For fungi, extensive studies have characterized the levels of both indoor and outdoor airborne fungi and their spores. More than viruses or bacteria, airborne fungi and their spores have been suggested to have the potential to enter a building that uses natural ventilation. Certain species (e.g., Aspergillus spp.) are also well-known, potentially life-threatening airborne contaminants when introduced to immunocompromised patients. Other fungi hazardous to the immunocompromised include Blastomyces spp., Coccidioides spp., Cryptococcus spp., and Histoplasma spp. Generally, fungi and their spores appear to be more resilient than viruses and bacteria, being able to withstand greater stresses due to dehydration and rehydration, as well as UV radiation.
Surfaces and persistence of microorganisms
Environmental surfaces were once thought to play a negligible role in the endemic transmission of nosocomial pathogens. However, recent data indicate that contaminated surfaces play an important role in the endemic and epidemic transmission of certain pathogens that cause healthcare-associated infections. Clostridium difficile, methicillin-resistant Staphylococcus aureus (MRSA), vancomycin-resistant enterococci (VRE), Norovirus, and multidrug-resistant (MDR) gram-negative rods including Acitonobacter baumannii share the ability to be shed from infected or colonised patients, survive on dry surfaces for extend periods, and are difficult to eradicate by cleaning and disinfection. For example, it is well described in the literature that MRSA is capable of surviving on surfaces from as little as 7 days up to 7 months, needing only 4 colony forming units (CFU) to cause an infection it still represents one of the biggest contributors of healthcare-associated infections (HCAIs) including sepsis, pneumonia, bacteremia and meningitis. Evidence that near-patient surfaces in hospitals could host MRSA was put forward by Boyce and colleagues in 1997. Their study also showed that health care staff could contaminate their gloves by handling or touching sites in close proximity to patients colonised with MRSA providing evidence of MRSA persistence on surfaces.
C. difficile spores can last in the environment or on surfaces for more than 5 months with an infectious dose of five spores only. Spores of C. difficile are durable and are resistant to usual cleaning methods. Contamination of the inanimate environment by C. difficile has been reported to occur in areas in close proximity to infected or colonised patients. Contamination rates have been as high as 58%; commonly affected surfaces and equipment with C. difficile include commodes, bedpans, blood pressure cuffs, walls, floors, washbasins, and furniture. Furthermore, VRE have been found in up to 37% of samples obtained from the environment and are most often found in association with diarrhoea. Samples were collected from the gowns worn by patients and health care workers, medical equipment, microsphere beds, and environmental surfaces. It was shown that VRE can survive on dry surfaces for up to 58 days on contaminated countertops.
In addition to bacteria, one recently published study reviewed the available data on the non-droplet routes of the spread of SARS-CoV-2 and other coronaviruses. The researchers stated that SARS-CoV-2 retained infectivity for up to 16 hours at room temperature. Coronaviruses and other viruses (including Influenza) can survive on both non-porous and porous surfaces, such as metals, fabrics, fibres (disposable handkerchiefs, handkerchiefs, cotton, polyester), plastics (light switches, telephones, latex, rubber and polystyrene), paper (also magazines, banknotes), wood, glass or eggs, feathers and soft toys. These, therefore, possess higher risks for patients and health staff. Also, Rotavirus is a well-known cause of outbreaks in daycare centres and health care settings, as it extensively contaminates and survives on surfaces, and may spread after contamination of toys shared among children. Norovirus has been the cause of diarrhoeal outbreaks on cruise ships, in hospitals, and in hotels. In 2002, a total of 9 outbreaks of norovirus on cruise ships were reported and outbreaks occurred on consecutive cruises, despite attempts to disinfect the ships.
 Waterborne pathogens
Waterborne pathogens
Waterborne diseases are those transmitted through the ingestion of contaminated water and water acts as the passive carrier of the infectious agent. Waterborne spread of infection by pathogenic agents depends on factors such as pathogen survival in water and the dose required for establishing infection in susceptible individuals. In addition to pathogen survival, latency (the period between pathogen excretion and acquisition of actual infectious power) and pathogen ability for multiplication in the environment are factors influencing the infective dose. The leading microorganisms that have been reported to cause water outbreaks include Legionella spp., Salmonella spp., Shigella spp., P. aeruginosa, Vibrio cholerae (cholera), and Campylobacter jejuni, with Legionella pneumophila being the leading cause of water outbreaks in hospitals and healthcare settings leading to Legionnaires’ disease. This is because temperature plays a significant role on the growth and survival of legionella. Hot water tanks, cooling systems, and towers, because of their heat-exchanging function, serve as bacterial “amplifiers”. Then, Legionella spp. are able to colonise all parts of internal distribution systems of hospitals, hotels, or buildings.
The number of worldwide outbreaks associated with waterborne pathogens was investigated in a systemic review by Castillo and colleagues (2015). From 1991 to 2002, 207 water outbreaks and 433,947 illnesses, associated with the protozoan agents Cryptosporidium, Naegleria fowleri, Giardia, and the bacteria Salmonella typhimurium, Vibrio cholerae, Legionella spp., Escherichia coli O157:H7 and Campylobacter jejuni, were reported in the United States of America. In the period of 1996 to 2006, 21 outbreaks and 507 cases of waterborne disease involving water not intended for dinking were reported. The etiologic agents were G. intestinalis, Legionella spp., E. coli O157:H7 and P. aeruginosa that resulted in acute gastrointestinal illness, acute respiratory illness, hepatitis, dermatitis and several deaths. From 2001 to 2006, Legionella spp., was responsible for 24 drinking water outbreaks, 126 drinking water-related cases and 12 drinking water-related deaths. In the Philippines, cholera is an endemic disease; it is estimated that 42,071 cases of cholera have occurred from 2008 to 2013. In 2012, 18 cases of cholera were reported by European Union (EU) countries. The United Kingdom reported 12 cases, France reported four cases, and Austria and Sweden all reported one case each.
Conclusion
Pathogenic microorganisms can be transmitted through different routes and can contribute to harmful community-and-hospital acquired infections. The survivability of these microorganisms relies on their microbial characteristics and their stability in different environments. As it was shown in numerous research papers, some microorganisms can have more than one vector of transmission and a good example of that is SARS-CoV-2, which was reported to be stable as an aerosol in the air environment, on dry surfaces and in water.





